

An anal fissure is a small tear or ulcer (open sore) in the skin just inside your anus (bottom). It causes severe pain and, sometimes, bleeding when you have a bowel movement (poo). Anal fissures often go away by themselves with some simple self-help measures. But if they don’t, there are several treatments that can help.
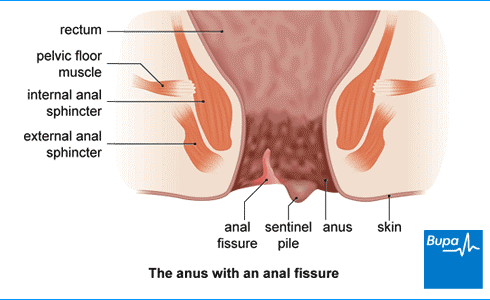
Anal fissures develop in the skin lining your back passage, just inside your anus (your anal canal). They usually develop towards the back of your anus, but you can sometimes get one at the front or even both together. If you have a condition that’s causing your anal fissures – for example, Crohn’s disease – you may get them anywhere around your anus.
If you’ve had an anal fissure for less than six weeks, it’s called an acute anal fissure. If it lasts for longer than six weeks, it’s known as a chronic anal fissure.
Anal fissures are common. It’s thought that around one in 10 people get one at some point in their life. Anyone can get an anal fissure, including children, but it’s most common in people aged 15 to 40.
For most people who develop an anal fissure, there isn’t any obvious reason why. This is called a primary anal fissure. It’s often thought to be the result of a hard or painful bowel movement damaging your anal canal. This can cause the muscles around your anus (the internal sphincter muscles) to spasm and tense up, making you more likely to tear. It also reduces the blood supply to the area, which makes it harder for any tears to heal.
Sometimes, there is a clear underlying cause for your anal fissure. This is known as a secondary anal fissure. Causes of secondary anal fissures include the following.
Anal fissure symptoms may include the following.
These symptoms may not always be due to an anal fissure. Other conditions, like piles (haemorrhoids) can cause similar symptoms. If you have any of the symptoms above, contact Doctor for advice. It’s always important to seek medical advice if you notice bleeding from your bottom.
Your doctor will usually be able to diagnose an anal fissure by asking about your symptoms and examining you. They’ll ask you to describe your symptoms and how long you’ve had them. They may also ask you about your health in general and your medical history.
Your doctor will examine you by asking you to lie on your side with your knees bent towards your chest. They’ll then gently part your buttocks to examine the area and see if there’s a fissure.
If there’s any uncertainty about what’s causing your symptoms or if initial treatments don’t help, your doctor may refer you to see a colorectal surgeon. This is a surgeon who specialises in conditions affecting your bowel and back passage.
Most anal fissures heal by themselves within six to eight weeks. There are a number of ways to help the fissure heal and to relieve your pain and discomfort. These include the following.
If your pain is particularly severe or your symptoms aren’t improving with self-help measures, there are a number of treatments your doctor may suggest.
The following medicines can help to relieve pain associated with an anal fissure or help the fissure to heal.
If other treatment options haven’t helped your anal fissure to heal or it keeps coming back, your doctor may refer you to a colorectal surgeon. Your surgeon will talk to you about what other options they may recommend. Options include the following anal fissure procedures.
You can reduce your risk of developing an anal fissure by preventing constipation. This is really important if you’ve already had an anal fissure that’s healed, as it can help to stop the fissure from coming back. You can help to prevent constipation by making sure you have a healthy balanced diet that contains plenty of fibre. It’s also important to make sure you’re drinking enough fluids and exercising regularly.
If you have another health condition that increases your risk of getting an anal fissure, speak to your doctor. They will tell you the best way to manage your condition and reduce your risk of getting an anal fissure.
An anal fissure is a small tear in the skin just inside your bottom. It can be very painful when you have a poo.
You’ll start to notice your symptoms improving as your fissure is healing. Your pain should lessen and if you had any bleeding, this should stop too. You should have a follow-up appointment with your doctor after six to eight weeks. This is to check that the fissure has healed.
Most anal fissures heal within six to eight weeks if you make changes to your diet and lifestyle and take medicines for pain relief. Sometimes, anal fissures heal more quickly than this. Sometimes, they last for longer and you may need further treatment.
You’ll usually experience severe pain when you have a poo if you have an anal fissure. But it’s also possible to have an anal fissure and not have any pain.
Anal fissures can be really painful but they’re treatable and aren’t usually a serious problem. But they can sometimes lead to other problems such as infection. If you avoid going for a poo because of a fissure, it can lead to faecal impaction. This is when you have a large blockage of poo in your bowels.
A chronic anal fissure is one that you’ve had for longer than six weeks. It might mean that you need specialist treatment or a procedure to get rid of your fissure.
The information and/or article is solely the contribution of Bupa, (hereinafter referred to as “Bupa UK”) a United Kingdom (UK) based healthcare services expert and is based on their experiences and medical practices prevalent in UK. All the efforts to ensure accuracy and relevance of the content is undertaken by Bupa UK. The content of the article should not be construed as a statement of law or used for any legal purpsoe or otherwise. Niva Bupa Health Insurance Company Limited (formerly known as Max Bupa Health Insurance Company Limited) (hereinafter referred to as “the Company”) hereby expressly disown and repudiated any claims (including but not limited to any third party claims or liability, of any nature, whatsoever) in relation to the accuracy, completeness, usefulness and real-time of any information and contents available in this article, and against any intended purposes (of any kind whatsoever) by use thereof, by the user/s (whether used by user/s directly or indirectly). Users are advised to obtain appropriate professional advice and/or medical opinion, before acting on the information provided, from time to time, in the article(s).
Please click on Agree button to be Redirected to BANCA Site.
Else click on close icon.

