

Chronic kidney disease is when your kidneys don’t work as well as they should. It’s a long-term condition which varies in how severe it is – from mild through to severe. Mild kidney disease is relatively common and can be managed successfully. Severe kidney disease is when your kidneys stop working (kidney failure) and this can be life-threatening.
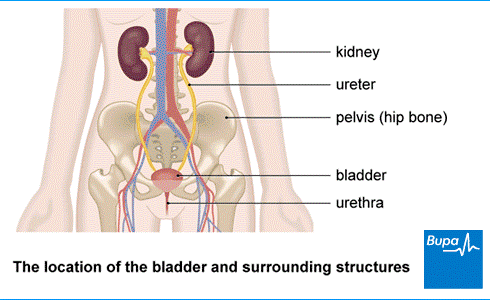
Your kidneys filter out waste products from your body and get rid of them in the form of urine. They also play a part in making red blood cells, balancing the amount of fluid in your cells and controlling your blood pressure. So, if your kidneys aren’t working properly, it can sometimes lead to serious long-term health problems.
If you have chronic kidney disease it means the condition has lasted for three months or longer. It’s a common condition and around one in 10 people have it. The chances of developing it increase as you get older and it’s linked to other conditions such as high blood pressure and type 2 diabetes, and being overweight.
Treating chronic kidney disease early and regularly monitoring it can help to slow down the development of the condition and prevent complications.
Chronic kidney disease is often diagnosed when you’ve already had it for some time, because there are usually no symptoms. It’s sometimes discovered when you have a routine blood or urine test for something else, or a check-up for another health condition, such as type 2 diabetes.
Symptoms usually only develop if you have severe kidney disease and kidney failure. Symptoms can be vague, but may include:
If you have any of these symptoms, speak to your doctor.
If you have a long-term health condition, such as high blood pressure, heart disease or diabetes, your doctor will do regular tests to check how well your kidneys are working. Your doctor will also test you for kidney problems if there is kidney disease in your family.
Your doctor will examine you and ask about any medicines you take and any other health problems. If your doctor thinks you may have kidney disease, you will have several tests. These can help to show how well your kidneys work, what the cause of any problem may be, and whether kidney disease has caused other health issues.
Your doctor will usually arrange for you to have these tests.
The results of these tests can help to show how severe the kidney disease is. See our FAQs about stages of kidney disease for more information. Depending on the results, your doctor may refer you to a nephrologist (a doctor who specialises in conditions that affect the kidneys).
You may also be asked to have an MRI or CT scan or a renal biopsy to find out the cause of your kidney disease. A biopsy is when a small sample of your kidney tissue is taken and sent to a laboratory for testing.
Chronic kidney disease is a life-long condition so the health professionals treating you will help you to self-manage as much as you can. That includes doing things like finding out about your condition, understanding your test results and what they mean and making changes to your lifestyle.
:There are many things you can do to help your kidneys work at their best. These include:
Non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or diclofenac, can affect how well your kidneys work, so don’t take them unless your doctor prescribes them. It’s a good idea not to take herbal medicines or protein supplements too.
People with chronic kidney disease can and do lead active and full lives. But living with chronic kidney disease can be challenging and difficult, and you’ll need to make changes to your lifestyle. If you’re finding it hard to cope or need support, ask your doctor or specialist nurse for help. They can refer you for one-to-one support or counselling. There are support groups for people with kidney disease where you can find information and support.
Chronic kidney disease can get worse over time, so treatment focuses on preventing this and helping you stay well. Your doctor will do regular check-ups and help you keep your kidneys working as well as possible, for as long as possible. You will also be given treatment to help prevent complications and manage other conditions such as high blood pressure.
The treatment you need will depend on how severe your kidney disease is.
Your doctor will ask you to take medicines to keep your kidneys working as well as possible and to prevent complications. You may be asked to take:
Some medicines can affect how well your kidneys work. Your doctor and pharmacist can check any other medicines you’re taking and tell you if you need to change them.
If you have any questions, ask your pharmacist or doctor for advice.
If you have severe kidney disease and your kidneys aren’t working, you’re likely to need either dialysis or a kidney transplant. You can also choose not to have either of these treatments and instead have your symptoms controlled to help you stay as comfortable as possible. Dialysis and kidney transplant aren’t suitable for everyone. Your doctor will talk about all the choices available for you and the pros and cons of each.
Dialysis acts like an artificial kidney by getting rid of waste and excess water from your blood. There are two types of dialysis.
A kidney transplant is when a kidney from a donor is put into your body. This can come from someone who is living or from someone who has died. If you have a kidney transplant, you’ll need regular check-ups for the rest of your life. You’ll also need to take medicines to stop your body rejecting the kidney.
Kidney transplants can be life-saving and can also improve the quality of your life because you won’t need regular dialysis.
Worried about your kidney condition?
Now you can consult with top nephrologist in India with our Second Medical Opinion Service available on Niva Bupa customer app.
The main causes of chronic kidney disease are diabetes and high blood pressure. Other possible causes include:
As kidney disease gets worse, you can develop complications, including:
If you have health problems which could lead to chronic kidney disease, such as diabetes or high blood pressure, it’s important to manage them well. If you get treatment for conditions like these early and keep them well controlled, it can reduce the likelihood of developing chronic kidney disease. Keeping to a healthy weight and not smoking can also help to prevent chronic kidney disease.
When you’re diagnosed, and as your condition changes, your doctor will use a ‘stage’ to describe how well your kidneys are working. The stages go from 1 to 5 and describe mild, moderate or severe kidney disease. Stage 1 is very mild kidney disease and stage 5 is severe kidney disease when your kidney isn’t working at all (kidney failure). Measuring these stages can help your doctor plan your treatment.
If you have mild-to-moderate chronic kidney disease, you can often be treated by a general physician. If you have more severe disease (stages 4 and 5), you’ll be treated by a nephrologist at a hospital.
This is difficult to answer, as how kidney disease develops is different for everybody. Not everyone will get to end-stage kidney disease.
Kidney disease doesn’t always get worse gradually, so it’s hard to predict when and if you’re likely to need dialysis or a kidney transplant. Mild chronic kidney disease is common and only a small number of people who have it will develop kidney failure.
If you’re diagnosed early, and have the right treatment and regular check-ups, you can prevent complications and slow down the development of the condition.
This is difficult to answer because everyone is different. Deciding which type of dialysis to have can be hard and you’ll need information and support from your doctor and nurse to help you choose. Both types of dialysis have pros and cons and you’ll need to think carefully about what will work best for you.
There are tools called decision aids that can help you to decide what’s right for you, and your doctor and nurse can give you more information and advice.
When you’re making a choice about treatment, there is a lot to consider. Here are some main things to think about.
The information and/or article is solely the contribution of Bupa, (hereinafter referred to as “Bupa UK”) a United Kingdom (UK) based healthcare services expert and is based on their experiences and medical practices prevalent in UK. All the efforts to ensure accuracy and relevance of the content is undertaken by Bupa UK. The content of the article should not be construed as a statement of law or used for any legal purpsoe or otherwise. Niva Bupa Health Insurance Company Limited (formerly known as Max Bupa Health Insurance Company Limited) (hereinafter referred to as “the Company”) hereby expressly disown and repudiated any claims (including but not limited to any third party claims or liability, of any nature, whatsoever) in relation to the accuracy, completeness, usefulness and real-time of any information and contents available in this article, and against any intended purposes (of any kind whatsoever) by use thereof, by the user/s (whether used by user/s directly or indirectly). Users are advised to obtain appropriate professional advice and/or medical opinion, before acting on the information provided, from time to time, in the article(s).
Please click on Agree button to be Redirected to BANCA Site.
Else click on close icon.

