

Ovarian cancer is when cells in or around your ovaries start to grow abnormally and out of control. You may also hear it called cancer of the ovaries.
Ovarian cancer is the third most common cancer in women in the India; around 50,000 women are diagnosed every year. It mostly affects women over 50, but younger women can get it too.
The ovaries are two small, oval organs which release an egg every month as part of a woman’s menstrual cycle (period). There are several types of ovarian cancer. These start in different parts of the ovaries and are treated in different ways.
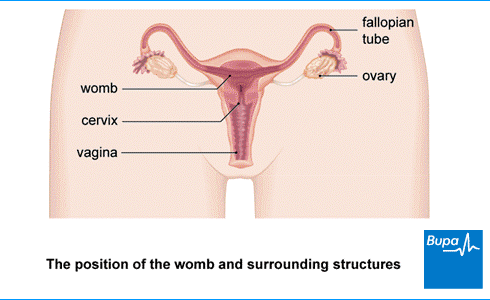
Sometimes, ovarian cancer can spread out of your ovary and fallopian tube, and more widely in your abdomen (tummy). More rarely, it can spread to other organs such as your liver, lymph nodes and lungs. This is known as malignant cancer.
Your doctor will tell you which type of ovarian cancer you have, and how that will affect your treatment options.
The most common ovarian cancer symptoms include:
Other symptoms include:
Many ovarian cancer symptoms are very vague and similar to symptoms caused by other, less serious conditions. And many women don’t have symptoms at all in the early stages of the disease. This means by the time many women see their doctor, the cancer is already at quite an advanced stage.
If you do develop any of the symptoms listed above, you’re getting them regularly and they last for longer than a few weeks, contact your doctor.
Your doctor will ask you about your symptoms and medical history. They will examine you by feeling around your abdomen (tummy) and pelvis. They may ask to examine you internally too. They’ll do this by gently feeling inside your vagina, to check your womb and ovaries for any lumps or swellings.
Depending on what symptoms you have and how long you’ve had them, your doctor may arrange for you to have a blood test. This is to check for a protein called CA125. A high CA125 level can be a sign of ovarian cancer, although other conditions can also raise your CA125 level. If your level of CA125 is found to be higher than normal, your doctor may also organise for you to have an ultrasound scan of your abdomen and pelvis.
Depending on your test results, your doctor may refer you to a gynaecologist (a doctor who specialises in women’s reproductive health). Sometimes, your doctor may refer you to a gynaecologist urgently (within two weeks), before conducting any further tests. They will then organise any tests and scans for you.
Your doctor will need to take tissue samples from the tumour, to confirm whether or not it’s ovarian cancer. These are usually taken when the tumour is removed during surgery – see our Treatment section below. Sometimes, your doctor may recommend a procedure to remove a sample (biopsy) of your ovary to test for cancer cells instead.
Your doctor will look at the tissue samples, along with the results of your blood and ultrasound tests to see how large your cancer is and how far it’s spread. Sometimes you’ll need other tests too, like a CT or MRI scan.
Finding out how far your cancer has spread is called staging. Staging can help doctors to estimate how your cancer is likely to progress, and the best course of treatment for you.
You should be offered genetic testing after you’re diagnosed with ovarian cancer, to check for faulty BRCA1 and BRCA2 genes. Having these faulty genes can increase your risk of breast and ovarian cancer. If you haven’t been offered testing, talk to your doctor about whether you’re eligible. Knowing whether you have the faulty BRCA genes may help your doctor to better plan your treatment. There are lots of things to think about before having a genetic test – your doctor will talk you through what’s involved.
A team of specialist doctors, including a gynaecological oncologist (a surgeon who specialises in cancers affecting the female reproductive system), will be involved in planning your care. What treatment they recommend will depend on the type of ovarian cancer you have, whether it’s spread, and if so, how far. They’ll talk to you about all the possible options, and anything that might affect your decision – including your general health and whether you plan to have children.
Almost all women with ovarian cancer have surgery. The aim of surgery is to remove as much of the tumour as possible. This is called ‘debulking’ surgery. It usually involves removing both ovaries, fallopian tubes and your womb (a total hysterectomy). Your gynaecological oncologist may also remove some surrounding tissue (biopsies) and nearby lymph nodes to help find out how far the cancer has spread.
If the cancer hasn’t spread beyond your ovary, and you want to have children in future, you may be able to just have the affected ovary and fallopian tube removed.
Most women with ovarian cancer also have chemotherapy. Chemotherapy is a treatment for cancer that uses medicines to destroy cancer cells. It usually involves having several doses of chemotherapy medicines at regular intervals over a period of weeks.
Most of the time, your doctor will offer you chemotherapy after surgery to destroy any cancer cells that weren’t removed by the operation. You might also be offered it before surgery to shrink your tumour, and make it easier to remove.
The exact chemotherapy treatment you’re offered will depend on the type and stage of your cancer. Your doctor will give you information on the type and course that’s best for you.
Radiotherapy uses radiation to destroy cancer cells. It’s not often used to treat ovarian cancer, but your doctor may offer it if your cancer comes back in another area of the body. It can also help to relieve symptoms such as pain, if other treatments are no longer possible.
These are newer medicines, including monoclonal antibodies and PARP (Poly ADP-ribose polymerase) inhibitors that specifically target cancer cells to stop them growing and multiplying. They may have fewer side-effects than traditional chemotherapy. You may be offered this treatment if you’ve been found to have a faulty BRCA gene, if your cancer is advanced, or if it’s come back.
You’ll have regular check-ups after your treatment has finished, to check how your cancer has responded and see if it comes back. It’s important not to miss these appointments, even if you’re feeling well. If your cancer has returned, your doctor will talk to you about any further treatment options you may be able to try.
It’s not clear exactly why some women develop ovarian cancer. But it is known that certain things can make you more likely to develop it. These include:
There are also certain things that reduce your risk of getting ovarian cancer. These include if you:
Stopping smoking and losing excess weight may help to reduce your risk of developing ovarian cancer, as well as a number of other cancers. This is also important for your general health. Making changes to your lifestyle can’t completely prevent ovarian cancer though, as there are many things – like your age and your genes that you can’t control.
If you have a strong family history (usually two or more close relatives who have had breast or ovarian cancer), your doctor may refer you to a genetic counselling clinic. Specialists at the clinic will be able to assess your risk and advise you on being tested for the BRCA1 and BRCA2 faulty genes. If you test positive for these genes, your doctor will talk to you about the options available to reduce your risk of both breast and ovarian cancer. For ovarian cancer, these include taking oral contraceptives and surgery to remove your ovaries and fallopian tubes (risk-reducing surgery).
Being diagnosed with ovarian cancer and facing treatment can be distressing for you and your family. An important part of cancer treatment is having support to deal with the emotional aspects and practical issues, as well as the physical symptoms. Specialist cancer doctors and nurses are experts in providing the support you need – make sure you talk to them if you have any concerns.
Talking to your family and friends can help them to understand what you’re going through and how you’re feeling. Organisations and support groups that specialise in ovarian cancer can also be a great source of information and support.
No. Unlike breast cancer and cervical cancer, there isn’t a national ovarian cancer screening programme at the moment. This is because tests to spot ovarian cancer at an early stage aren’t good enough yet.
There is a blood test for ovarian cancer – it looks for a substance called CA125. This can be high if you have ovarian cancer. But your levels of CA125 can also be high for many other reasons – for example, if you have fibroids or endometriosis. And it also doesn’t always pick up on cancer if you have it. Because of this, the test isn’t used to look for ovarian cancer in women who don’t have symptoms.
If you’re worried about your risk of ovarian cancer, talk to your doctor. They may refer you to a local genetics service for genetic screening if you have a strong family history. See our section on Prevention above for more information.
In some women, it’s possible that initial treatment with surgery and chemotherapy will successfully remove all of the cancer, and they’re then said to be ‘in remission’. This means that there’s no sign of the cancer coming back. This is more likely if your cancer is diagnosed at an early stage.
In other women, the initial treatment may not be able to completely get rid of the cancer, or the cancer may return later on. This is more likely if the cancer has already spread beyond your ovary by the time it was diagnosed. There are additional treatment options for ovarian cancer that has spread or come back, including targeted therapies.
These aim to control the cancer for as long as possible. See our Treatment section above for more information.
Many studies have looked to see if there’s a link between using talcum powder and getting ovarian cancer. The suggestion is that, if you use talcum powder around your genital area, the powder could travel up inside to reach your ovaries. The theory is that it could then cause irritation, which may eventually trigger cancerous changes over time.
The results from these studies have been mixed. Some find that using talcum powder increases the risk of ovarian cancer; some find no link. There isn’t enough evidence to confirm a clear link. Even if talc does increase the risk of ovarian cancer, the risk is thought to be very small. Other factors, such as age, weight and smoking are much more important. See our section on the Causes of ovarian cancer above for more information.
Taking the contraceptive pill at any point in your life reduces your chance of getting ovarian cancer. The contraceptive pill works by stopping you from ovulating every month, which is known to reduce your risk of ovarian cancer. The longer you take the pill for, the bigger the reduction in your risk. Your risk is halved if you take it for five years or more. Once you stop taking the contraceptive pill, it carries on protecting you from ovarian cancer for several years afterwards too.
Taking the contraceptive pill might not be suitable for everyone. Generally, the benefits of taking it outweigh any possible risks, but some people are at higher risk of certain important side-effects. Talk to your doctor or nurse about whether it’s suitable for you.
www.targetovariancancer.org.uk
www.ovacome.org.uk
www.macmillan.org.uk
www.cancerresearchuk.org
The information and/or article is solely the contribution of Bupa, (hereinafter referred to as “Bupa UK”) a United Kingdom (UK) based healthcare services expert and is based on their experiences and medical practices prevalent in UK. All the efforts to ensure accuracy and relevance of the content is undertaken by Bupa UK. The content of the article should not be construed as a statement of law or used for any legal purpsoe or otherwise. Niva Bupa Health Insurance Company Limited (formerly known as Max Bupa Health Insurance Company Limited) (hereinafter referred to as “the Company”) hereby expressly disown and repudiated any claims (including but not limited to any third party claims or liability, of any nature, whatsoever) in relation to the accuracy, completeness, usefulness and real-time of any information and contents available in this article, and against any intended purposes (of any kind whatsoever) by use thereof, by the user/s (whether used by user/s directly or indirectly). Users are advised to obtain appropriate professional advice and/or medical opinion, before acting on the information provided, from time to time, in the article(s).
Please click on Agree button to be Redirected to BANCA Site.
Else click on close icon.

